FAQs
Pediatric dentists are the pediatricians of dentistry. A pediatric dentist has two to three years of specialty training following dental school, and is the primary and specialty oral care provider for infants and children through adolescence, including those with special health needs.
The American Academy of Pediatric Dentistry recommends that a child's first visit to the dentist should occur by 12 months of age. This visit will enable the dentist to evaluate your child and introduce you to proper oral hygiene. Diet, fluoride, finger and pacifier habits, and tooth eruption will be discussed to ensure optimal dental health. Discussing the prevention of oral infections and the prevention of dental/facial injuries is the cornerstone to the year-one visit.
The American Academy of Pediatric Dentistry recommends that you brush children’s teeth with a fluoride toothpaste twice a day (for children 2 years or older.) Floss children's teeth once a day. Visit your pediatric or general dentist regularly. Ensure that fluoride is consumed through drinking water, fluoride products, and fluoride supplements. Apply sealants to the chewing surfaces of permanent molars. Snack moderately, no more than twice a day. It is best to snack on foods with minimal or no sugar content. Fresh fruits and vegetables make great snacks.
Set a good example. Make good oral health a family effort. Show children that daily brushing and flossing, limited snacking, and regular dental checkups are necessary for good oral health. Support your child when he or she is able to brush and floss on his or her own, assisting and performing spot checks as needed.
While good oral hygiene is of utmost importance in the prevention of cavities, lack of a proper diet can have a tremendous impact on a child’s cavity rate. Limit not only the quantity of consumed sugary foods and beverages, but also the frequency throughout the day. Cavity formation is a process. When sugar comes in contact with teeth, the cavity process can begin. The more times in a day that we consume sugar, the more at risk we are for developing cavities. By nature, many children like to snack throughout the day, and many of these foods, including juices, are loaded with sugar. Even some” healthy” foods can be very high in sugar content, including granola bars, cereal, and chocolate milk. Check the nutritional label if you are uncertain as to how much sugar a food item contains. Have your child drink plenty of water following snacking.
The chewing surface of teeth is most at risk for developing cavities and is least benefited from the protective effects from fluoride. Sealants are adhesive coatings that are applied to the chewing surfaces of teeth and are very effective in preventing tooth decay. Current research shows that for children under the age of fifteen, 80% of cavities develop on the chewing surfaces of molars. Food and plaque accumulate in the tiny grooves of these chewing surfaces, which are normally very difficult to keep clean. In fact, toothbrush bristles may not effectively clean these grooves. Sealants prevent cavities by ‘sealing’ off these grooves, preventing bacteria from causing cavities in these areas.
Amalgams or silver fillings are used to restore or "fill" decayed areas in teeth. Although amalgam fillings have a scientifically proven history of safety and effectiveness in restoring teeth, we do not use silver amalgam filling at Kids Smile.
Composites or tooth colored fillings are used to “fill” areas of decay and restore fractured teeth in which cosmetic appearance is important. The shade of the restoration material is matched as closely as possible to the color of the natural tooth. This is typically the restoration of choice, unless treatment conditions dictate the use of another material.
Stainless steel crowns are silver colored "caps" used to restore teeth that are too badly decayed to hold fillings, need a nerve treatment, or have concerns about durability. Crowns with white facings can be used on front teeth.
This procedure is a nerve treatment in which the sick portion of the tooth nerve is removed and medicine is placed in order to avoid extracting the tooth.
A pulpectomy is necessary when the nerve of the tooth is dead. The entire infected pulp is removed and medication is placed in the root canals.
Nitrous Oxide (laughing gas) is ALWAYS administered with oxygen. Nitrous oxide is a safe gas and is 100% exhaled by the patient. The combination of nitrous oxide and oxygen, inhaled by your child during the restorative appointment, is used to relax a mildly anxious child. Nitrous Oxide/oxygen also acts to minimize discomfort during dental treatment. Your child does not fall asleep and can effectively communicate with the dentist. Your child should be able to return to normal activities upon leaving the dental office; however please limit the amount of physical activity of your child immediately following treatment.
A space maintainer is used to hold space for a permanent tooth when a baby tooth has been prematurely lost. If space is not maintained, teeth on either side of the missing tooth can drift into the space and prevent permanent teeth from erupting.
Although primary teeth are often called baby teeth, the first tooth is usually lost around age six, while primary molars are normally lost between 10 to 13 years of age. Primary teeth are necessary for proper chewing, speech, development of the jaws, and aesthetics. Taking care of primary teeth is important for proper oral function, to prevent cavities on permanent teeth, and to prevent pain and infections from occurring.
Parents are invited back to accompany their child during the initial examination and during any treatment your child may receive. Parents are always allowed to accompany any child three years of age or younger. We do encourage parents, however, to allow children to enter the treatment area alone if we think your child will behave better and have a more positive experience. Please let our receptionist know if you request special accommodations. If your child needs to be sedated for treatment or needs hospital dentistry care under general anesthesia, parents are asked not to accompany their child. There are no exceptions to this rule.
If your child has a dental emergency during office hours, please call our office as soon as possible. We will see your child immediately. If it is an after-hours emergency, a pager number will be given on the answering machine. If you are unable to reach a member of our team, proceed to the emergency room to ensure treatment in a timely manner. If your child lost consciousness related to the injury, call 911.
Treating a permanent tooth that has been “knocked out” within the first few minutes is critical for the survival of that tooth. If a permanent tooth is knocked out, gently rinse, but do not scrub the tooth under water. Replace the tooth in the socket if possible. If this is impossible, place the tooth in a glass of milk or a clean wet cloth and come to the office immediately. If the tooth is fractured, please bring in any pieces you can find. If a baby tooth is knocked out, we do not recommend putting the tooth back in the mouth.
Our normal schedule may be delayed in order to accommodate an injured child. Please accept our apologies in advance should an emergency occur during your child's appointment.
Yes. Some children with disabilities are more susceptible to tooth decay, gum disease, or oral trauma. Certain medications, special diets, or oral habits detrimental to dental health are common among special-needs children. If preventive dental care is started early and followed conscientiously, every child can enjoy a healthy smile. Learn more about our dental service for special needs children.
A first dental visit (Well-Care visit) by age one will be the beginning to a lifetime of good dental health. We will obtain a full medical history, perform an examination of your child's teeth and gums, and then develop a preventive care plan specifically designed for your child's needs.
Yes! Your child will benefit from the preventive approach recommended for all children: effective daily brushing and flossing, moderation of snacking, and proper amounts of fluoride. Adequate oral home care takes minutes a day and will prevent many dental problems. Regular professional cleanings and fluoride treatments will help prevent or help catch problems early if they should arise.
Specialty education in pediatric dentistry provides additional training that focuses specifically on the care for children with special health-care needs. Our office is designed to be physically accessible for special-needs patients.
For the average child, the ideal time for orthodontics will be just before the last of the primary/baby teeth naturally fall out. This will usually occur at approximately eleven. However, there are circumstances in which children benefit from phase I or interceptive orthodontics. For this reason, the American Association of Orthodontists typically recommends that children have a screening appointment with an orthodontist at age seven. At this time, the orthodontist will discuss future treatments, including the timing of such treatment.
Athletic mouth protectors are soft plastic mouth guards made specifically for your child's teeth. They protect the teeth, lips, cheeks, and tongue. They can help protect children from such serious head and neck injuries as concussions and jaw fractures. Increasingly, organized sports are requiring mouth guards to prevent injury to their athletes. Research shows that most oral injuries occur when athletes are not wearing mouth protection.
The majority of children stop sucking on thumbs, fingers, pacifiers, or other objects on their own between two and three years of age without any harm being done to their teeth or jaws. However, children that repeatedly suck on a finger, pacifier, or other object over long periods of time may cause the upper front teeth to tip toward the lip or not come in properly. We will carefully monitor the direction of tooth eruption into the mouth. Often, problems that arise related to oral habits will correct themselves if stopped in a timely manner. However, the longer the habit persists, the more likely it will cause a permanent malformation of the jaw and related skeleton.
The majority of children stop sucking habits on their own. Some children may need the help of their parents. When your child is old enough to understand the possible results of an oral habit, we will encourage your child to stop. We will explain to him or her what happens to the teeth if she or he doesn't stop. It is very important to get children to want to stop and to realize that it is a part of growing up. This will greatly increase their chances of terminating the habit. Once your child wants to stop, a reward system and earnest reminders will help him or her accomplish the goal. If all other options have been exhausted, we will discuss with you the use of a fixed dental appliance to exhaust the habit.
General anesthesia provides a way to effectively complete dental care in an operating room facility in a hospital. Usually only children with severe anxiety and/or severe tooth decay are recommended for general anesthesia. Typically, these children are very young or have compromised health concerns.
YES. While normal risks are always present with surgery, a pediatric anesthesiologist will put your child to sleep. This person is responsible for delivering the general anesthesia, monitoring the child, and overseeing the medical care of the child. Many precautions are taken to provide safety for the child during general anesthesia care. Anesthesia personnel, who are trained to manage potential complications, monitor patients closely during the general anesthesia procedure. We can discuss the benefits and risks involved with general anesthesia and why it is recommended for your child's treatment.
Usually, your child's surgery is performed as an "outpatient" basis. Surgery will occur in the morning and your child will be discharged in the afternoon to return home. A physical examination is required prior to a general anesthesia appointment to complete dental care. This physical examination provides information to ensure the safety of the general anesthesia procedure. We will advise you about any evaluation appointments that may be requested.
Prior to surgery – Gently discuss with your child about the appointment; this may reduce anxiety. Explain to her or him that he or she is "going to go to sleep when her is his teeth are being fixed." Avoid using words like "hurt."
Eating and drinking – You will be informed about food and fluid intake guidelines prior to the appointment. It is absolutely essential that no food or liquids be consumed after midnight the night before surgery.
Changes in your child's health – If your child is sick or running a fever, contact us immediately! It may be necessary to arrange another appointment.
Usually, children are tired following general anesthesia. You may wish to return home with minimal activity planned for your child until the next day. After that, your child will usually be able to return to his or her routine schedule.
Conscious sedation is a way of using medication to relax a child without the loss of consciousness.
Dr. Bagheri may recommend conscious sedation for children with severe anxiety and/or the inability to cooperate during treatment. He will discuss the pros and cons of sedation on a case-by-case basis.
Conscious sedation aids in calming a child so that he or she can accept dental treatment in a more relaxed state. This can prevent injury to the patient and provide a better environment for delivering quality dental care. sedation dentistry for kids
Advanced education in pediatric dentistry offers advanced training to administer, monitor, and manage sedated patients. Dr. Bagheri is certified in CPR/Pediatric Advanced Life Support and exceeds the required standards of care in his monitoring and emergency equipment.
Extractions:
The gauze needs to stay in place with biting pressure for 15-30 minutes. This will reduce the amount of bleeding.
Give your child the appropriate dose of children's Tylenol, Motrin, or Advil when you take the gauze out (NO aspirin). Your child should only need this for approximately 12 to 24 hours. If pain persists beyond 48 hours, please call our office.
Allow your child to begin eating only soft foods (mashed potatoes, macaroni and cheese, yogurt, jell-o, etc.) for the first 24 hours. Please avoid sharp, crunchy foods because the area may be sensitive. Encourage plenty of liquids (water, soups, etc.). You can transition to a regular diet as the gum tissue begins to heal.
NO spitting or drinking through a straw or "sippy" cup for 24 hours. The force can start the bleeding again.
A clean mouth heals faster. Gentle brushing around the extraction site can be started immediately along with warm salt water rinses (1/4 teaspoon to a glass of water) to aid with any discomfort.
Activity may need to be limited.
Your child's cheek, lip, and tongue will be numb for approximately 1-2 hours. Please be very careful that your child does not bite at his or her cheek or scratch this area. As this area "wakes up," it may feel funny. A self-inflicted bite injury is the most common post-op complication. Please monitor your child closely.
Care of the Mouth after Local Anesthetic
Your child has had local anesthetic for his or her dental procedure. If the procedure was in the lower jaw, the tongue, teeth, lip, and surrounding tissue will be numb. If the procedure was in the upper jaw, the teeth, lip, and surrounding tissue will be numb.
Often, children do not understand the effects of local anesthesia, and may chew, scratch, suck, or play with the numb lip, tongue, or cheek. These actions can cause minor irritations or can be severe enough to cause swelling and abrasions to the tissue. Please watch your child closely for approximately two hours following the appointment. It is our recommendation to keep your child on a liquid or soft diet until the anesthetic has worn off.
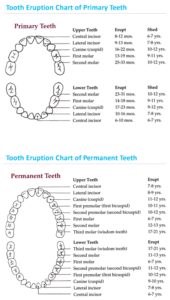
Children’s teeth begin forming before birth. As early as 4 months, the first primary (or baby) teeth to erupt through the gums are the lower central incisors, followed closely by the upper central incisors. Although all 20 primary teeth usually appear by age 3, the pace and order of their eruption varies.
Permanent teeth begin appearing around age 6, starting with the first molars and lower central incisors. This process continues until approximately age 21.
Adults have 28 permanent teeth, or up to 32 including the third molars (or wisdom teeth).